Author: Paul E. Enochs, MD, FACS, FASMBS
When many of us think about robotics, our minds may drift to images of automobiles and airplanes transforming into fighting defenders to save our world from attacking invaders. Perhaps, instead, we think about the futuristic world of the Jetsons, where our mechanized friends help us get ready in the morning, clean our house, and aid us throughout the day. Yet despite these images, the reality is that robotics exists in the present-day world and has already started to enter every part of our daily lives. The surgical field is no exception.
Techniques for bariatric surgery – past
Fifty years ago, surgery was performed primarily through a large open incision, allowing a surgeon to directly visualize a patient’s internal anatomy and touch the organs with their hands. Three decades ago, a laparoscopic, endoscopic, and videoscopic revolution began in gynecology, continued into general surgery, and eventually spread to every specialty.
With these new minimally invasive techniques, surgeons were able to utilize small incisions to place a scope through which the patient’s internal anatomy could be viewed on a video monitor. At the same time, their hands could control instruments that went through the small incisions to work on the organs. This novel technique rapidly changed surgery by decreasing patient morbidity, allowing for less pain, more rapid recovery, reduced infection risk, shortened hospital stays, and quicker returns to regular activity.
In adopting this new procedural approach, surgeons had to develop a new skill set to overcome some of the shortcomings of this new field. The field of view was limited while surgeons had to learn a new method of depth perception and hand-eye coordination to overcome the two-dimensional visualization. In addition, new techniques had to be developed to overcome the changes in proprioception, dexterity, and range of motion.
As the years passed and technology advanced with better scopes and instruments, these limitations did not disappear but were overcome as surgeons honed and expanded their new set of skills. Eventually, the majority of procedures done in the thoracoabdominal cavity had been attempted and were being performed primarily through a minimally invasive technique.
Techniques for bariatric surgery – current
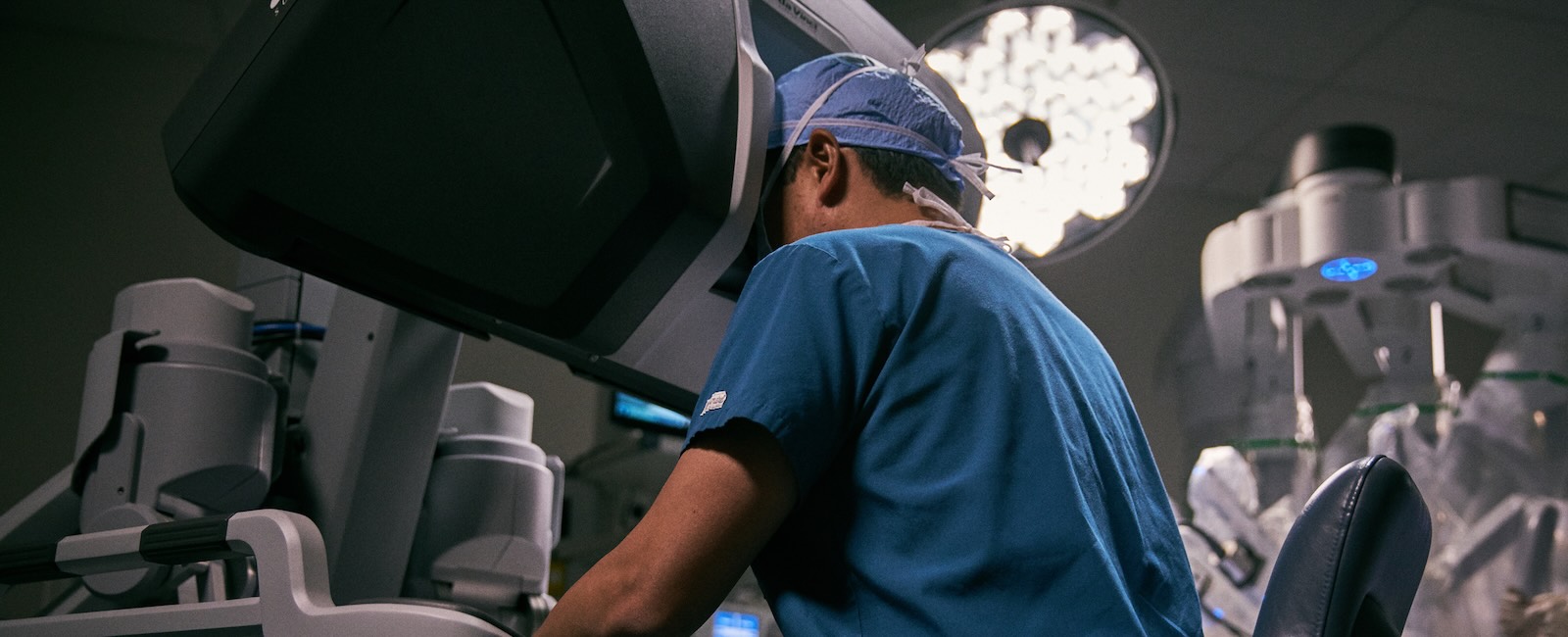
In 2000, the FDA approved the da Vinci robotic surgical system for widespread use in general laparoscopic surgery. Before this time, robotics had been evaluated for use in the military and cardiac surgery. This new technology allowed surgeons to have three-dimensional magnified visualization and an increased range of motion due to wristed instrumentation.
The surgeon’s hands now controlled robotic arms, which, in turn, moved instruments through small incisions to touch the organs. For the first time in the history of surgery, the need for a surgeon’s hands to be in direct contact with the patient’s organs wasn’t a requirement, but instead separated by an electromechanical interface. This advancement in technology has enabled more refined and precise movements, thereby causing less trauma to the abdominal wall, target organs, and tissues. In addition, single-incision technology and remote surgery have now become more of a real possibility.
Robotics in the surgical fields
Not all surgical fields immediately adopted this new surgical approach. Urology became the first specialty to adopt the new robotic technology readily. By 2009, nearly 80% of all radical prostatectomies were being done through the robotic approach. Gynecology became the next specialty to adopt the robot for wide use in hysterectomies and other pelvic procedures. Despite the acceptance of this robotic technology by different specialties, the field of general surgery and, by extension, bariatric surgery was somewhat slower to adopt and readily recognize its usefulness. The reason for this is varied.
One reason was that, at the time, more than 90% of all bariatric procedures were performed using the minimally invasive approach. Today, most bariatric surgeons are trained on a robotic platform, and many (even today) are skilled in laparoscopic techniques and have mastered advanced laparoscopic maneuvers. In contrast, when robotic surgery was applied to prostatectomies and hysterectomies a couple of decades ago, the majority of these procedures at the time were done through an open approach. As such, a greater benefit in those fields was perceived. In addition, it is only relatively recently that vessel sealing and stapling technology, integral to most bariatric procedures, has become available on the robotic platform. Finally, critics of robotics in the bariatric field point to a myriad of topics, including a new learning curve with longer surgical times and a perceived increase in costs, as reasons to avoid change.
Benefits of robotics to bariatric surgery
Understanding the above critiques and perceptions, the question arises as to what benefit robotics provides to bariatric surgery. There are several. It is important to realize that the robotic platform is not a new surgical procedure but a technology with the potential to enhance feedback and information to the operator, thereby improving the skills of a skilled surgeon. All of the bariatric procedures from sleeve gastrectomy and gastric bypass to duodenal switch and SADI are now most often performed robotically.
A review of the published literature has shown that the use of robotics in these procedures is a safe and reasonable option. In fact, several studies have shown a lower complication rate with the robotic platform, including leaks, bleeding, and stricture. Although operator dependent, as with all surgery, this can be attributed to the better three-dimensional magnified visualization and increased dexterity associated with the robotic platform.
Another benefit of robotics is better ergonomics and decreased surgeon fatigue. This can be very beneficial in the higher BMI patients with thicker abdominal walls, where the ergonomics of traditional laparoscopy can be physically demanding and lead to surgeon fatigue. In addition, the increased range of motion and improved optics allow for more meticulous, precise dissection and suturing, which can be integral to revisional bariatric cases with their extensive adhesionolysis and need for difficult intracorporeal sutured anastomoses. In these complex bariatric procedures, the robotic technology also enables real-time assessment of tissue perfusion through the use of fluorescence imaging. Knowledge of the blood supply to a revised anastomosis or gastric pouch can be integral in the prevention of staple line breakdown and leak.
Finally, when evaluating the abilities of the robotic platform in bariatrics, it is imperative to remember that this is an evolving technology. Advancements in laparoscopy over the last half-century were made possible through improvements in many of the instruments we use today, and robotics is no different. Whether it is single-site platforms, natural orifice surgery, telesurgery, real-time assessment of tissue thickness and perfusion by the staplers, radiographic image integration into the surgical field, or increased haptic feedback, once the fundamental techniques of the robotic platform are learned, it can serve as a foundation on which these new technologies are built.
Over time, these and as-yet-undiscovered technologies could provide an exciting vehicle to transform the way we care for our patients in bariatric surgery.